|
Sterility Assurance
Levels Required For Medical Devices & Sterilization
Methods
Many of the procedures and applications require devices
to be in temporary or permanent contact with a patient’s
skin, tissue, blood, or other parts of the body. Such
devices should not cause infection to the patient from
microbiological contamination or residues.
Contamination from microorganisms can come from various
sources that could include the raw material from
suppliers, the manufacturing process and the storage,
handling and distribution processes.

Many devices need to be packaged and sterilized, either
before distribution or before use. Examples of such
devices are surgical gloves, clean room garments,
specimen cups, wound care products, sutures, needles,
syringes, catheters, drain bags, IV bags, fluid delivery
systems, dialysis equipment, implants, surgical
instruments, dental instruments, surgery supplies, and
combination products. Devices for such applications
should be sterile before use to ensure that the
microbiological contamination is minimized. The
purpose of sterilization is to inactivate the
microbiological contaminants and thereby transform the
nonsterile medical devices into sterile products.
Fig below lists some of the different types of
microorganisms and their resistance to disinfection and
sterilization.
Most resistant
|
Most resistant
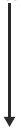
Least resistant |
• Prions
• Bacterial spores
• Mycobacteria
• Small, nonenveloped, nonlipid viruses
• Gram-negative bacteria
• Fungi
• Large, nonenveloped, nonlipid viruses
• Gram-positive bacteria
• Vegetative bacteria
• Medium-sized lipid enveloped viruses |
Adapted from Favero MS, Bond WW Chemical Disinfection of
Medical and of Medical and Surgical Material. In:
Disinfection, Sterilization and Preservation, 5th
Edition Phila: Lippincott Williams & Wilkins 2001 pp.
881-917
ISO 11139 details sterilization process standards and
provides a vocabulary of terms used in sterilization of
medical devices.3 EN 556-1 is the harmonized European
standard specifying requirements for designating a
terminally sterilized device as sterile.4 It has also
been adopted in a number of countries outside Europe,
for example, Australia and China. EN 556-1 specifies
that a probability of a viable microorganism on a device
of 10-6 or less (e.g., 10-7 ) has to be achieved in
order to designate a terminally sterilized medical
device as sterile. EN 556-2 is the harmonized European
standard specifying requirements for designating an
aseptically processed device as sterile.5
The sterility of any product is defined by the
probability of a viable microorganism on the product
after it has been sterilized. This probability is
referred to as a Sterility Assurance Level (SAL) which
is defined as the probability of a single viable
microorganism occurring on an item after sterilization.3
The SAL is normally expressed as 10-n and is
quantitative value to assume sterility. SALs of 10-3 or
10-6 are the most frequently used values for
sterilization. The lower the SAL, the higher the
sterility of the medical device or material. The
probability of a single viable microorganism occurring
on an item after sterilization can never be reduced to
zero (i.e. 100% assurance level).
Sterility Assurance Level (SAL)
Types of Medical Devices requiring different levels
of Sterility Assurance levels ( Either 10-6 and 10-3 )
Illustrative List Of Products with Sterility
Assurance Level (SAL), SAL = 10-6 0r less
A Products and materials intended to come into
contact with breached skin or compromised tissue:
• Catheters
• Cannulas
• Wound dressings
• Prefilled syringes
• Incise drapes
• Surgical Instruments
• Ventilators
B Invasive Products and materials that come into
contact with sterile tissue:
• Lead extraction devices
• Surgical instruments
• Ultrasound probes
• Biopsy probes
• Endoscopes
• Bronchoscopes
C Products and materials that come into contact with
sterile fluid pathways:
• Fluid delivery administration sets
• IV tubing
• Dialysis tubing
• Syringe needles; syringes
• Blood collection devices
• Endoscopes
D Surgically implanted devices:
• Stents
• Cardiac Leads
• Implanted infusion pumps
• Implanted orthopedic devices
• Sutures
• Intraocular lenses
• Surgical meshes
E Cell-based and tissue-based devices
Illustrative List Of Products with Sterility
Assurance Level (SAL), SAL = 10-3
A Products not intended to come into contact with
breached skin or compromised tissue:
• Blood collection tubes, specimen containers, culture
media devices
• Surgical drapes and gowns,
• Medical equipment
B Products incapable of achieving an SAL 10-6 by any
sterilization method:
• Porcine heart valves
Methods used to sterilize medical devices include moist
heat (steam) or autoclaving, dry heat, radiation, EtO
gas, vaporized hydrogen peroxide, and other
sterilization methods like chlorine dioxide gas,
vaporized peracetic acid, and nitrogen dioxide. EtO
sterilization comprises 50% of the global sterilization
market, followed by gamma radiation (40.5%), e-beam
(4.5%), and other methods of sterilization like steam
autoclaving, hydrogen peroxide, etc., (5%).
Sterilization procedure includes always some
disadvantages due to the simple fact that there is a
certain amount of energy necessary to destroy living
germs, even those, which are specialized on harsh living
conditions. On the other hand, a sterilization procedure
should be as fast and reliable as possible and has no
impact on plastic materials as well. Interesting
emerging technologies for medical device sterilization
might be:
• Plasma beam sterilization
• Hydrogen beam sterilization
• X-ray beam Sterilization
• Electro-beam sterilization |
